Every year the UK’s kidney doctors and nurses come together for the British Transplant Society meeting when we look at the achievements of the past year, and our hopes for the year to come. It is also a great opportunity to showcase some of the research advances from Guy’s and St Thomas’ Trust.
I continue to be in awe of these advances and our contributions, which are making real improvements to our patients’ lives.
Here are my top four advances in transplant research from our hospital
Number 1:
Warm kidney perfusion
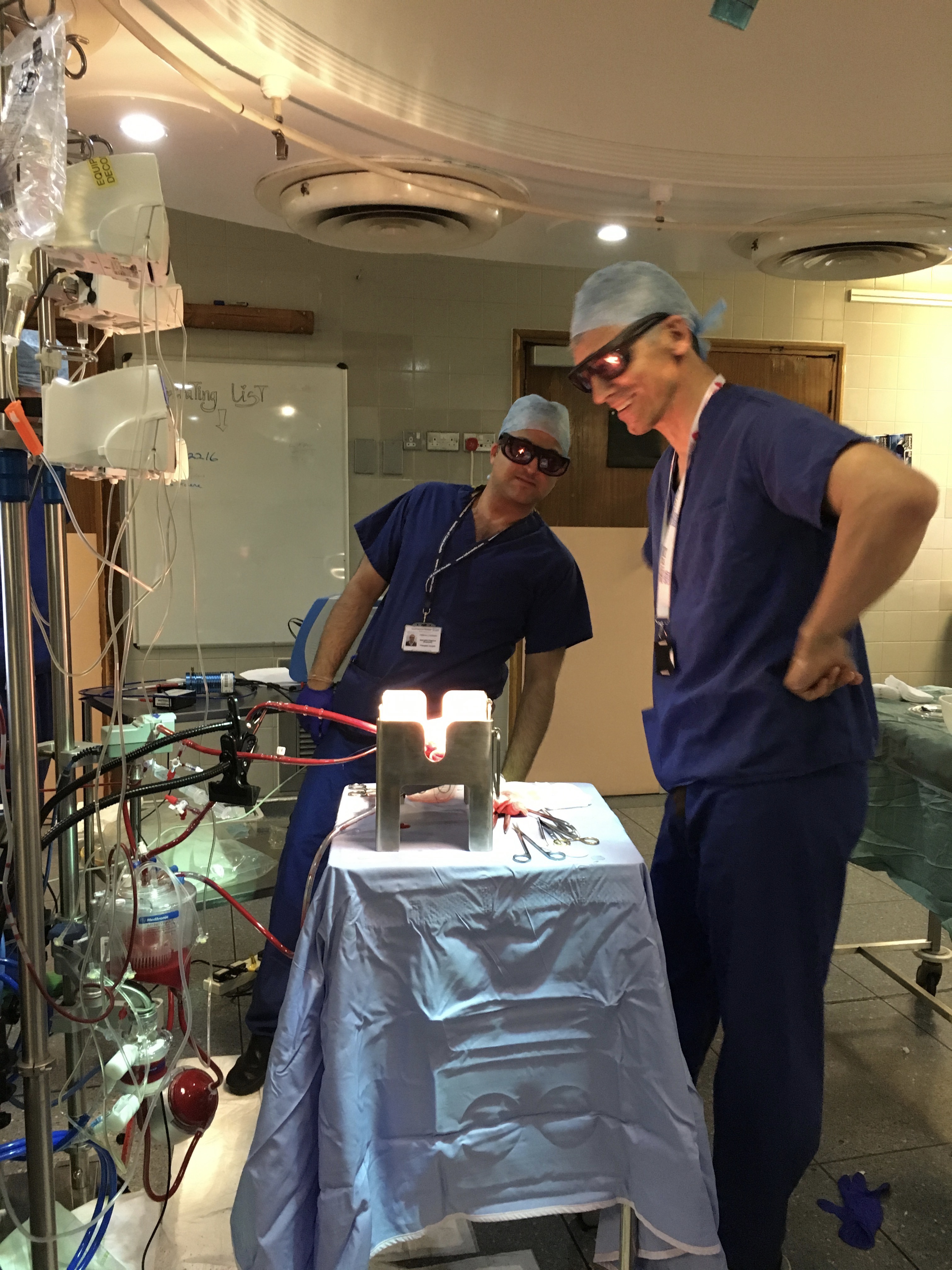
Traditionally after a kidney is donated, it is stored in ice before it is inserted into the new recipient. For the last 60 years this has been a good way of ensuring the kidney stays viable while we get ready to do the transplant operation. However, kidneys stored in this way can be a little slow to ‘wake up’ after the operation, and some people still need a few sessions of dialysis until the kidney starts working. Keeping kidneys warm may be a way of reducing ‘sleepy kidney’.
We have therefore been trialling a machine that pumps kidneys with oxygen and blood at body temperature (known as ex vivo normothermic perfusion; EVNP). This research is being led by Mr Chris Callaghan, consultant transplant surgeon. Research into this alternative form of organ storage has been funded by GSTTKPA, and so far about 50 GSTT patients have received kidneys using this new technology.
We are so grateful to everyone who has volunteered for this research at the time of their transplant and we look forward to letting you know the results soon!
Number 2:
Monitoring blood flow in kidney transplants
After the transplant operation, the doctors and nurses have to make sure that the blood flow to the new kidney remains strong. An ultrasound scan is requested whenever we need to check that the kidney is receiving plenty of blood.
Our research fellow Mr Pankaj Chandak has been developing a new probe that will provide live, real-time information on how much blood the transplanted kidney is receiving. This probe will sit next to the kidney after the operation and alert the team if blood flow goes down. Early diagnosis of poor blood flow will allow us to fix the problem quicker. It should also reassure the surgeon and patient when the kidney is doing well. Pankaj is working hard to get this new technology ready for patients in the next few years.
Number 3:
HIV-positive donors
Previously, HIV-positive people could not donate their kidneys. Given the shortage of kidneys, could these people be considered for donation to recipients with HIV? With promising results from South Africa, Guy’s Hospital embarked on the challenge of finding organ donors with the same subtype of HIV as potential recipients.
All the necessary approvals were gained, and Guy’s became the first UK centre to transplant kidneys from HIV-positive donors. With more kidney donors, this
is one strategy to reduce the transplant waiting list.
Number 4:
Robotic kidney transplantation
Sounding like something out of a science-fiction movie, surgeons at Guy’s are using a robot to both remove a kidney from the donors and transplant it into the recipient. Using a 3D camera, the surgeon controls four robotic arms to perform the operation. The value is faster patient recovery, as it is a less invasive form of surgery. Professor Nizam Mamode, lead transplant surgeon at Guy’s Hospital, became the first in the UK to transplant a kidney using the robot. As our experience grows, more patients may benefit from this novel technology.
The team at Guy’s and St Thomas’ will continue to try and improve the care we give, and we thank GSTTKPA for their ongoing support.
By Benedict Phillips
Clinical Research Fellow, Specialist Registrar in Transplantation, Guy’s & St Thomas’ NHS Foundation Trust